SARS-CoV-2 Spike Protein Causes Blood Clots
One of the remarkable observations about SARS-CoV-2 infection is the clinical manifestation of venous and arterial thrombosis.
Multiple studies have described thrombotic complications of the infection including stroke, myocardial infarction, systemic arterial embolism, and deep venous thrombosis with pulmonary embolism. In my practice I have seen virtually every one of these complications. De Michele and colleagues studied patients with COVID-19 in 2020, before there were vaccines for the population.[i]
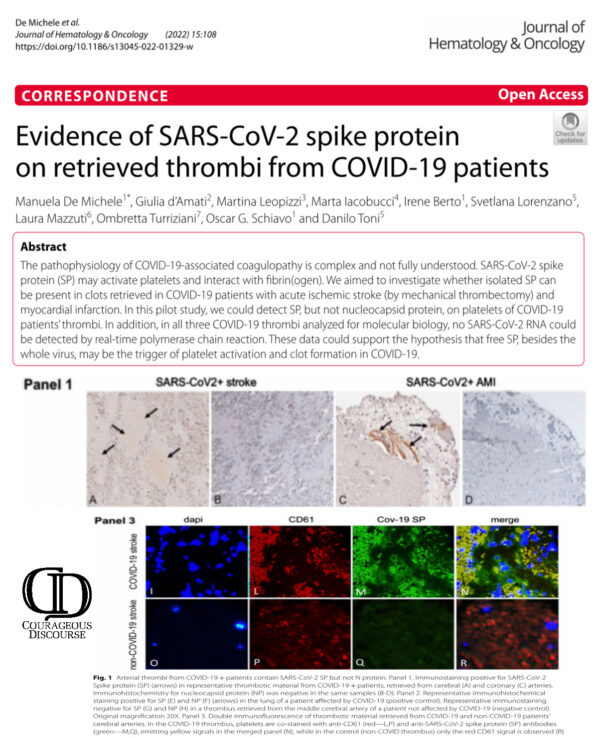
They found SARS-CoV-2 Spike protein directly attached to platelets within the blood clots retrieved from patients. Importantly, there was no evidence of the entire virus. This suggests the Spike protein disassociates from the virus and becomes its own clot forming missile within the human body. I could anticipate that mRNA, adenoviral DNA, and Spike protein antigen-based vaccines act the same way by generating free Spike protein within plasma which is able to circulate and participate in the development of blood clots.
Virchow’s triad is an axiom in medicine that says blood clots require three elements:
1) injury to the vessel wall,[ii]
2) stasis of blood, and
3) a hypercoagulable state.
SARS-CoV-2 Spike protein is known to damage the endothelial lining of capillaries and blood vessels and cause hypercoagulability. Stasis of blood is inherent in various venous beds such as the cavernous sinus of the brain, portal vein in the abdomen, pelvic veins, and in the lower extremities of immobilized patients. Thus for venous thromboembolic cases Virchow’s triad is fulfilled.
The arterial emboli take more explanation suggesting atherosclerotic plaque instability, platelet aggregation, and Spike protein driven hemagglutination, fibrin deposition, and progressive clot formation occur. No matter what the sequence, in the setting of SARS-CoV-2 infection, blood clots can be attributed to Spike protein.
Large questions remain:
1) for how long after infection can Spike protein trigger atherosclerotic cardiovascular events (heart attack and stroke) and venous thromboembolism?
2) what is the initial risk period and accumulated risks of additional infections and or COVID-19 vaccination?
3) what are the best methods for screening, detection, diagnosis, prognosis, and management?
Disclaimer: Articles are for informational purposes and are not a substitute for individualized medical advice. Please consult a trusted professional for personal medical advice, diagnoses, and treatment.
About the Authors:Dr. Peter A. McCullough, MD
Dr. Peter McCullough is a practicing internist, cardiologist, epidemiologist managing the cardiovascular complications of both the viral infection and the injuries developing after the COVID-19 vaccine in Dallas TX, USA. He has dozens of peer-reviewed publications on the infection, multiple US and State Senate testimonies, and has commented extensively on the medical response to the COVID-19 crisis in TheHill, America Out Loud, NewsMax, and on FOX NEWS Channel.
John Leake
John Leake studied history and philosophy with Roger Scruton at Boston University. He then went to Vienna, Austria on a graduate school scholarship and ended up living in the city for over a decade, working as a freelance writer and translator. He is a true crime writer with a lifelong interest in medical history and forensic medicine.








Comments
Post a Comment