Bruce Patterson Long Hauler Protocol: Has Bruce Patterson Cracked Long COVID?
Bruce Patterson MD is a former Stanford researcher with quite a record. The former Medical Director of Diagnostic Virology at Stanford University Hospitals and Clinics, Patterson has co-authored around 90 papers – most prior to 2011 – at about the time he left the University and created the incellDx diagnostic laboratory. Over the past ten years, incellDx has focused mostly on cancer screening and has produced products to test for HPV, CMV, antibodies, and others. Over the past two years, though, Patterson has jumped back into the publication field, co-authoring 7 papers on COVID-19 with more to come.
Update: Desperate Patients Are Shelling Out Thousands for a Long Covid Cure. Is It for Real?In June of 2020, Patterson reported that he’d identified the cause of the so-called “cytokine storm” in COVID-19.
“When we were developing a cytokine quantification assay for possible COVID trials in China, we discovered that infected patients had consistently high levels of CCL5/RANTES in plasma which in some cases was 100 times normal depending on the severity of the disease.”Patterson and incellDx filed a patent in June 2020 for its CCL5/RANTES diagnostic test for COVID-19, Patterson reported. In October, incellDx reported that it was collaborating on a COVID-19 clinical trial using Pfizer’s CCR5 antagonist Maraviroc – a key part of Patterson’s long-COVID protocol.
Patterson is all over social media. His YouTube interviews and presentations have garnered over 400,000 views over the past year. ABC News just led with a story: “EXCLUSIVE: Lab discovers root cause of confusion, fatigue experienced by COVID ‘long haulers‘
Patterson has become a kind of a sensation … and why not? He’s credible, claims to be studying the largest cohort of long haulers (thousands) in existence, and believes that not only has he found the cause of long COVID, but that he’s put together a treatment regimen that works. No new drugs are needed – everything is off the shelf. It almost couldn’t be better.
How excited are people? One doctor on YouTube is so sure that Patterson has got it right that he recommended that he be nominated for a Nobel Prize. That’s a bit much for a hypothesis and treatment regimen which hasn’t been independently validated yet, but it does portray some of the excitement Patterson has generated.
Patterson, incellDX and the Coronavirus
As noted, it all began in the summer of 2020 when Patterson and incellDX found abnormal levels of cytokines – signaling fire in the body. Patterson’s first COVID-19 paper in May 2020 found a “profound elevation of plasma IL-6 and CCL5 (RANTES)” in 10 critically ill COVID-19 patients. It was followed in January 2021 by a paper showing that a COVID patient with a poor T-cell response was still shedding the virus 90 days after becoming infected. Next, Patterson and his team found that a CCL5 blocker called leronlimab might be a good drug to try in COVID.
Patterson’s two major papers, “Immune-Based Prediction of COVID-19 Severity and Chronicity Decoded Using Machine Learning“, and “Persistence of SARS CoV-2 S1 Protein in CD16+ Monocytes in Post-Acute Sequelae of COVID-19 (PASC) Up to 15 Months Post-Infection” – the second an unreviewed preprint – showed up in June of this year.
Immune Cells and Cytokines
On the face of it, the first paper didn’t seem revolutionary at all. This type of study – which assessed the immune cell subsets and 14 cytokines – has been done many times in chronic fatigue syndrome (ME/CFS). (In a talk, Patterson noted that he’d winnowed down the cytokines from about 150 possible factors to 14.) The study involved a mishmash of 224 acute COVID-19 and long-haul COVID-19 patients and 24 healthy controls.
The study found that CCL5/RANTES, IL-2, IL-4, CCL3, IL-6, IL-10, IFN-γ, and VEGF were all significantly elevated (all P<0.001) while GM-CSF and CCL4 were significantly reduced in COVID patients in general.
Next, they used machine learning to develop immunotypes pertaining to each type of COVID patient and found long-haul COVID patients were characterized by increased IFN-γ and IL-2, and reduced CCL4 production.
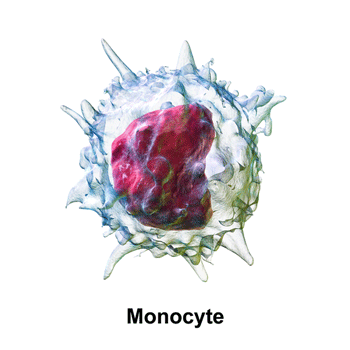
Monocytes are the key immune player in Patterson’s long COVID hypothesis (.com staff (2014). “Medical gallery of Blausen Medical 2014”. WikiJournal of Medicine 1 (2). DOI:10.15347/wjm/2014.010. ISSN 2002-4436.)
In a rather torturous sentence, the authors proposed that “the inflammatory context created by these cytokines that leads to T cell activation is not enough to generate an adequate anti-viral response without the proper recruitment signals to attract activated T cells.” My take on that is that they believe that the inflammatory context created by the cytokines, combined with inadequate T-cell recruitment, did not create an “adequate antiviral response” in the long-COVID patients.
The T-cells were apparently raring to go, but the low CCL4 levels failed to attract enough of the T-cells to the virus to successfully fight off the virus.
T-cell exhaustion has been speculated in ME/CFS, but possibly because many T-cells never found their way to the virus, there was no sign of T-cell exhaustion. The reduced number of total T regulatory cells, on the other hand, failed to keep the immune response in check. This was demonstrated by increased levels of B-cells, and in particular, high levels of a monocyte subset.
The authors proposed that high IL-2 levels promoted B-cell proliferation and differentiation, but high IFN-y levels may have damped down B-cell activity.
With the T, and perhaps B-cells, at least somewhat out of action, the immune system threw monocytes into the breach. It was the monocytes that caused the lung damage sometimes found in acute COVID – and which Patterson et al. believe are causing long COVID.
The big takeaway seemed to be that the acute and long COVID patients had trouble fighting off the virus, allowing it to persist longer in them. The immune system compensated for the lack of a proper T and B-cell response by calling in a particular subset of monocytes with some interesting properties indeed.
The Second Paper
The second paper, “Persistence of SARS CoV-2 S1 Protein in CD16+ Monocytes in Post-Acute Sequelae of COVID-19 (PASC) Up to 15 Months Post-Infection“, tied their hypothesis together.
As noted, it wasn’t just the monocytes – it was a particular kind of monocyte – that was increased in both acute and long COVID-19.
First, the group looked for evidence that COVID-19 had infected the monocytes in both acute and long-COVID patients and found evidence of some infection but not a lot. COVID-19 replication does not appear to be the problem.
When they used antibodies to look for evidence of coronavirus proteins in the monocytes, though, they found them – in spades. Seventy-three percent of the “non-classical” monocytes in long-COVID patients carried the coronavirus proteins. (They used another test – Ultra-High-Performance Liquid Chromatography – to largely confirm the results.)
These types of monocytes have often been thought to be anti-inflammatory, but recent studies show that they can, in some situations, produce pro-inflammatory cytokines. They’re mostly involved in “trash cleanup”, and the antiviral response. Interestingly, they appear to be unique in the patrolling behavior they exhibit around the blood vessels.
The authors believe these monocytes were drawn to coronavirus-infected cells in the blood vessels, where they ingested them, and then put a coronavirus protein on their surface to alert the immune system. The problem in long COVID occurs when they are drawn to the blood vessels and injure them, or cause the blood vessels to inappropriately dilate.
These nonclassical monocytes are the only monocytes to carry the CX3CR1 receptor, which when it binds to fractalkine, turns on an anti-apoptotic protein that allows the monocytes to survive longer than usual. It also causes the monocytes to revert from their anti-inflammatory state, and start pumping out pro-inflammatory cytokines.
These are important steps as most monocytes die within a few days, and having very long-lived (up to at least 16 months) coronavirus protein-carrying monocytes is a crucial aspect of Patterson’s hypothesis. Patterson also needs these monocytes to attack the blood vessel walls.CX3CR1 is also an important player in getting the monocytes to engage in their vascular patrols, and deleting CX3CR1 has been shown to reduce their patrolling behavior.
Monocytes carrying the SARS protein and endothelial cells are producing high levels of CCL5/RANTES – a chemokine that draws the monocytes cells to the endothelial cells. Patterson reported that CCL5/RANTES was upregulated in 80% of long haulers. Once at the endothelial cells, the monocytes bind to them via fractalkine – a kind of immune Velcro.
The monocyte binding also triggers the production of VEGF – which Patterson reports is elevated in almost all long haulers. VEGF then dilates the blood vessels causing, Patterson thinks, feelings of fullness in the head, migraines, and perhaps cognitive problems.
The many different symptoms that arise depend on where in the body the blood vessels – including those in the brain – get hit.
He also believes that monocytic reservoirs of infection were established early in people who later became long haulers. Those COVID-19 patients treated with steroids might inadvertently have allowed those reservoirs to be established. (If true, that’s something that the NIH-funded studies should readily pick up.)
Diagnosis
Patterson reported they were able to use the immune data to create a “long-hauler index”, and successfully diagnose virtually all the long-COVID patients from the healthy controls. That’s a good step forward, but numerous studies have been able to successfully differentiate people with ME/CFS from healthy controls. That, in itself, is not that big of a deal.
Treating
Patterson, an MD, reported that they started treating long-COVID patients in September 2020. Patterson’s protocol has two main goals:
- Use CCR5 antagonists to reduce CCL5/RANTES levels, and therefore prevent the monocytes from getting to the blood vessels.
- Damp down the CX3CR1/fractalkine pathway in order to turn off the long term monocyte survival mechanism that’s allowing them to survive longer than usual. Over time, the monocytes carrying the coronavirus protein will die off.
The Protocol
The treatment protocol is remarkably brief – just 4-6 weeks. First, immune labs are taken and then 3 drugs are given. (The fact that none of these drugs have been used in ME/CFS should remind us how vast the medical drug toolkit is and how many possibilities it holds.)
Drugs

Patterson uses different drugs to prevent monocytes from getting to the blood vessels
- CCR5 antagonist – Maraviroc (Selzentry (US), Celsentri (EU)) is an antiretroviral drug used in combination with other drugs to treat HIV. (HIV can use the CCR5 receptor to enter the cell). Its efficacy against the coronavirus is also being explored. Maraviroc also stops monocytes from moving around the body in response to CCL5/RANTES – a chemokine which is produced in endothelial cells. Maraviroc comes with plenty of warnings, including a black box one, but Patterson says it is safe – and has two papers coming out on it. Most long haulers are on for 2-4 weeks and the longest has been 8 weeks. Maraviroc, he said, was incredibly effective in relieving tinnitus and brain fog and typically did so in 3-5 days. He said “we see it (tinnitus) a lot, and treat it a lot and are very good at eliminating it.”
- Statins – by inhibiting fractalkine, it stops the monocyte cells from attaching to endothelial cells on the blood vessels.
- Ivermectin -an immunomodulator and anti-parasitic drug is used because of its persistent antiviral properties. It also affects cell membranes. A meta-review of 11 randomized Ivermectin COVID-19 trials found a significant reduction in hospitalization and and 56% reduction in death. Many of the trials were not peer-reviewed, and a wide range of doses was used.
The majority of patients see some improvement in two weeks. After 4 weeks, more improvement is seen and the labs are repeated to see if the immune system has been restored. Weeks 4-6 typically see the immune systems returning to normal and people getting back to normal lives with most of their symptoms gone. The 5-10% of the symptoms left at this point were, he thought, probably to being sedentary or bedridden for so long. He slowly starts them off on exercise during this period.
Serial monitoring of some patients has shown that the levels of the monocytes carrying the SARS-CoV-2 protein are declining. He believes eventually these cells will get cleared, and when they do, the disease is apparently over. (One doctor did refer to possible blood vessel damage if the condition is present for too long).
Many people, he said, have had success with the protocol, and he could count on the fingers of his hands the number of people who have not responded.
Post-Vaccination Long Haulers?
Patterson reported he’s assessed from 100-200 people who came down with what looks like long COVID in the months after being vaccinated. Machine learning analyses indicated it was a quite heterogeneous group, but with one exception (no elevations of VEGF), immunologically, they looked like long haulers and the long-hauler treatment worked for them.Chronic Fatigue Syndrome (ME/CFS), Fibromyalgia and Lyme Disease
Patterson clearly feels for the long haulers saying that it’s “gut-wrenching” that “it’s taken us this long to recognize long COVID and treat it aggressively”. “The economic hardship of long COVID” he said, “is mind-boggling…”

Patterson believes similar processes are at work in ME/CFS, FM and Lyme disease and promised to move aggressively on them
Lives disrupted, jobs lost, health gone, relationships impacted – it’s all true – yet it’s a walk in the park compared to what the really long haulers – the people with ME/CFS – have experienced.
Patterson has not forgotten them, though, and said he plans to aggressively expand into chronic fatigue, fibromyalgia, and post-Lyme disease, where Patterson believes similar processes (i.e. some sort of ongoing antigen stimulation) are in play.
He suggested that in Lyme disease, pieces of the cell membrane of bacteria may remain in the blood for months/years.
The consistent cytokine/chemokine pattern found in his long haulers has not shown up in ME/CFS, however. A few studies have highlighted only a few of his markers. One metareview found increased L-2 and IL-4 levels in ME/CFS and another study found reduced levels of VEGF.
A recent review of cytokine levels in 15 ME/CFS studies of overall moderate quality didn’t find any consistency in cytokine results.
“The findings of this study indicate that of the 64 cytokines analyzed, none appear to differ with any consistency between CFS/ME/SEID patients and healthy controls, in either serum or other physiological fluids, despite comparability between each study’s analytical methods…despite the consistent data, the findings of this review are inconclusive as to whether cytokines play any definitive role in CFS/ME/SEID, other than provide some evidence of a concurrent inflammatory process.”
Nor have altered monocyte levels been found in ME/CFS. Out of the many gene expression studies, only one found evidence of increased monocyte expression.
Of course, ME/CFS is much more heterogeneous than long COVID. Different pathogens or different triggers may elicit different responses; i.e. some other form of antigenic stimulation – if it’s present – may, and probably is, be tweaking the immune systems of different patients. One very nice intersection between Patterson’s and recent ME/CFS hypotheses and findings is the focus on the blood vessels.
If Patterson’s hypothesis wins out in long COVID, one would think it would spur quite a search into the antigenic stimulation possibly underway in ME/CFS, FM, Lyme disease, and others.
Cracking long COVID?
IncellDx has clearly gone all-in on long COVID. (Because it’s a diagnostic laboratory it stands to do very well selling its test kits. It should be noted that Patterson’s findings – while exciting – have not been validated by outside researchers. Some may remember the XMRV testing that didn’t work out in MECFS.)
It’s rare, though, that you see this kind of engagement. An online Chronic COVID Diagnosis and Treatment Center has been created “…in partnership with prominent research facilities, clinicians, and medical laboratories”. Long-COVID patients can get the cytokine/chemokine incellKine test kits here. A telemedicine appointment is then scheduled, after which incellDx will apparently match you up with a doctor. Check out FAQs here.
IncellDx is all in on long COVID. It’s recruiting patients and doctors, publishing papers, creating apps, and branching out into other countries. Time will tell if it’s cracked long COVID.
Patterson reported they are working with a hundred physicians to support them in writing the needed prescriptions and managing their patients. (Doctors can become a part of their network of treating providers here.)
IncellDx has a pilot study going in the UK and is moving into Central and South America. IncellDx is also creating an app and watch that will help track symptoms, HR, HRV, meds, and labs. They’re also looking at post-vaccination illnesses. Studies from the Patterson team are continuing to come out. Patterson wants to move into ME/CFS, FM and Lyme.
It’s no wonder that Patterson recently said he’s working from the time he wakes until his head hits the pillow at night.
Treatment studies, including at some point, placebo-controlled treatment studies are obviously crucial. With hundreds of doctors trying his protocol Patterson is potentially gathering a lot of data. Patterson’s immune findings also need to be validated by other labs. A lot needs to happen before we can say Patterson has cracked long COVID.
People who’ve been around ME/CFS have seen promising hypotheses and even good data fall by the wayside before. The body, as Ron Davis has reminded us, is a tricky, tricky thing. Certainly, it seems a bit early for long COVID to fall (I expected it to take a couple of years) but hopefully Patterson’s cracked it in record time – and will take his shot at ME/CFS and other diseases. Time, of course, will tell.
Check out Patterson’s attempt to take over a company making a CCR5 inhibitor.
Original Article: https://www.healthrising.org/blog/2021/07/21/patterson-cracked-long-covid/
Editor's Note: COVID-19 is a highly dynamic topic. Please refer to the latest Treatments for COVID long hauler syndrome.








.png)
Comments
Post a Comment