Long Covid patients, in search of treatment, turn to private company
A full two years into the coronavirus pandemic, long-haul Covid patients remain sick and in desperate search of answers. They've lost jobs. They've lost their sense of self. Many say they have lost faith in the medical community.
Despite multiple studies, the launch of dozens of specialized long Covid clinics and $1.15 billion in federal funding for the National Institutes of Health to study the condition, there remains a dearth of proven treatments for people who are suffering from lingering illness after their infection.
"There is no one right answer for many of our patients," said Dr. Ben Abramoff, director of the Post-COVID Assessment and Recovery Clinic at Penn Medicine, which has seen more than 1,100 long Covid patients.
Compounding the problem is a lack of consensus on how to define long Covid, according to a commentary published Tuesday in the Annals of Internal Medicine from researchers at UCLA Health and the David Geffen School of Medicine in Los Angeles.
"We do not know what constitutes long Covid or how to formally diagnose it," the authors wrote. "An improved understanding of this condition is needed to provide appropriate care for our patients."
Most hospital-affiliated clinics, including Penn Medicine, treat patients with a variety of medical teams, including counselors, cardiologists, pulmonologists, physical therapists and immunologists.
But it can take months to get an appointment, and many patients say finding treatment for long Covid can be time-consuming and draining. That gap has allowed private companies to step in with promises of relief.
The most well-known is IncellDx, a California-based company that said it has accomplished three key goals specific to long Covid: a diagnostic test, a treatment plan, including an HIV drug and cholesterol-lowering medications, and a way to show patients that the treatment is working.
Critics counter that there are no simple blood tests or widely accepted biomarkers to determine whether someone has long Covid. Even at highly respected clinics, treatment regimens vary widely and doctors don't offer cures. Instead, most treat the symptoms in an effort to get patients back to some sense of normalcy.
The myriad symptoms that come with long Covid make it difficult to come up with a standardized treatment.
The illness, characterized by lingering symptoms weeks to months after an infection, can take on many forms. Some people have daily migraines. Others lose their train of thought midsentence. Some can no longer walk the short distance from their front door to their mailbox.
Long waits and long-term plans
In the past two years, scores of long Covid treatment clinics, typically affiliated with hospitals or medical research centers, have opened nationwide.
When Laurie Bedell, 42, of Pittsburgh, first sought treatment, she waited nearly eight months for an appointment at the Cleveland Clinic more than 130 miles away. When her health insurance refused to pay for the visit, she was forced to find a doctor closer to home.
"I waited months and got nothing done," she said. "I'll probably be waiting months again for hopefully somebody in Pittsburgh."
The wait is not easy for patients like Bedell — a former nursing director who, before Covid, was accustomed to working out for two hours, six days a week. Now, she said, "I physically can't function. I have a walker. I can't drive because I have cognitive dysfunction, and my vision's constantly blurry."
At the Covid Activity Rehabilitation Program at the Mayo Clinic in Rochester, Minnesota, where doctors have treated hundreds of people with long Covid, patients are advised to take their recovery slowly.
"Patients, when they get sick, they just so want to get back to normal life," said Dr. Greg Vanichkachorn, an occupational medicine specialist who heads Mayo's post-Covid program.
But plunging into normal activities is exhausting after so much time being sick, and can lead to flare-ups and fatigue that feel like a relapse.
"The body just can't handle that," he said. "Pacing is so important — helping people understand the importance of proper pacing from the very get-go so they don't get into this situation."
Vanichkachorn, like many long Covid clinicians, focuses on treating symptoms. He often prescribes a blood pressure medicine called midodrine and a steroid called florinef in an attempt to improve blood flow in the body. Physical therapy is also important, he said, to help keep muscles toned and as strong as possible.
Hinda Stockstill, 35, of Cincinnati, said her long Covid has improved following a combination of treatments from both her family doctor and physicians at the Cleveland Clinic's post-Covid treatment center.
She has undergone physical and occupational therapy, and has taken an antiviral called acyclovir and fluvoxamine, which treats depression.
"It didn't cure me completely," Stockstill said. "I still do have some days where I'm just so tired, I can barely get up. But they're fewer and far between."
"Most patients have improvement over time," Abramoff said. But about half "don't get back to 100 percent."
No answers yet at the NIH
The cause of long Covid is still unknown. Why do some people infected with the coronavirus recover, while others continue to be plagued by symptoms?
Several theories exist. A recent study suggested that the immune systems in some people do not react appropriately to the virus, and don’t trigger the correct antibodies. Another study found that the coronavirus may reactivate the Epstein-Barr virus, which causes mononucleosis, or be linked to Type 2 diabetes.
In February 2021, the NIH energized legions of long-haulers with the allocation of more than $1 billion for long Covid research through 2025.
"We all were really hopeful — like, OK, finally something is happening!" Bedell said. She was part of a focus group of long Covid patients from which the NIH sought guidance as it began its flagship research project called Researching COVID to Enhance Recovery, or RECOVER.
FLCCC I-Recover Protocol
- Ivermectin: 0.2mg/kg body weight. Once daily for 1 week. Discontinue after 2 - 4 weeks if all symptoms have resolved. A repeat course is recommended in those who respond poorly or relapse once the treatment is stopped. The anti-inflammatory properties of ivermectin may mediate this benefit. (Find a Doctor)
- Prednisone: 10–15mg daily for 3 weeks. Taper to 10mg for three days, then 5mg for three days and then stop.
- Low dose naltrexone (LDN): Begin with 1 mg daily and increase to 4.5mg as required. May take 2–3 months for full effect.
- Omega-3 fatty acids: Vascepa, Lovaza or DHA/EPA 4g per day. Omega-3 fatty acids play an important role in the resolution of inflammation by inducing resolvin production. [Ref, Ref]
- If symptoms do not improve after 1–2 weeks continue steroids, omega-3 fatty acids and Naltrexone and add second line medications.
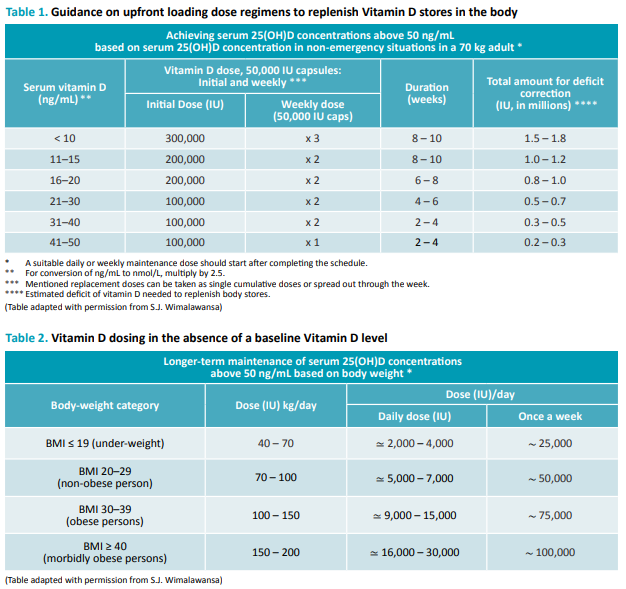
- Vitamin D: The majority of those with post-COVID-19 syndrome continue to have hypovitaminosis D. See tables 1 or 2 for vitamin D supplementation.
- Fluvoxamine (low dose): 25mg once daily. Stop if the symptoms increase. Caution with the use of other antidepressants and psychiatric drugs. Taper and discontinue once symptoms improve.
- Atorvastatin: 20–40mg once daily. Caution in patients with Postural Orthostatic Tachycardia Syndrome (POTS); may exacerbate symptoms.
- Maraviroc: 300mg PO twice a day If 6–8 weeks have elapsed and significant symptoms persist, consider either getting an InCellDx test to assess long hauler index profile prior to initiating or can consider initiating empirically. Note maraviroc can be expensive and it has risk for significant side effects and drug interactions.
- Curcumin: has anti-inflammatory and immunomodulating properties and has been demonstrated to repolarize macrophages.
- Nigella Sativa: which like curcumin has anti-inflammatory and immunomodulating properties.
- Vitamin C: 500mg BID (vitamin C inhibits histamine and repolarizes monocytes). [Ref]
- Melatonin: 2–8mg at night (slow release/extended release) with attention to sleep hygiene. Increase dose from 1mg as tolerated (may cause severe nightmares at high dosages).
- Kefir, probiotic yogurt and/or Bifidobacterium Probiotics (e.g., Daily Body Restore) together with Prebiotics (e.g. XOS Prebiotic, Bio Nutrition Pre-Biotic) to normalize the microbiome. Prolonged dysbiosis has been reported following COVID-19 infection.
- Behavioral modification, mindfulness therapy and psychological support may help improve survivors’ overall well-being and mental health.
- Luteolin 100–200mg day or Quercetin 250mg day (or mixed flavonoids). Luteolin and quercetin have broad spectrum anti-inflammatory properties. These natural flavonoids inhibit mast cells, and have been demonstrated to reduce neuroinflammation.
- H1 receptor blockers (for mast cell activation syndrome): Loratadine 10mg daily, or Cetirizine 5–10mg daily, or Fexofenadine 180mg — daily.
- H2 receptor blockers (for mast cell activation syndrome): Famotidine 20–40mg, or Nizatidine 150mg — twice daily as tolerated.
- Montelukast: 10mg/day (for mast cell activation syndrome). Caution as may cause depression in some patients.
- Anti-androgen therapy: Spironolactone 50–100mg twice a day, and Dutasteride 1mg daily.
Main Reference: https://www.nbcnews.com/health/health-news/long-covid-patients-private-company-help-rcna9035?








.png)
Comments
Post a Comment